Laryngeal Stenosis: A Complex Post-COVID-19 Complication
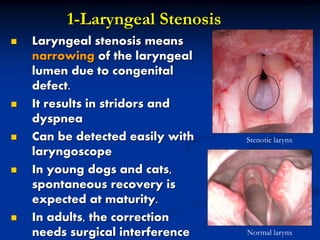
- Medical researchers and clinicians are identifying laryngeal stenosis—a narrowing of the airway in the larynx—as a complex and often overlooked complication following severe cases of COVID-19.
- Laryngeal stenosis occurs when the airway becomes constricted due to the formation of scar tissue or inflammation.
- The narrowing of the larynx is rarely a direct result of the SARS-CoV-2 virus itself, but rather a consequence of the life-saving measures employed in intensive care units.
Medical researchers and clinicians are identifying laryngeal stenosis—a narrowing of the airway in the larynx—as a complex and often overlooked complication following severe cases of COVID-19. While the pandemic’s primary focus remained on pulmonary failure, the physical trauma associated with critical care interventions has left a subset of survivors with significant airway obstructions.
Laryngeal stenosis occurs when the airway becomes constricted due to the formation of scar tissue or inflammation. In the context of the COVID-19 pandemic, these conditions are frequently linked to the prolonged use of endotracheal tubes in patients who required mechanical ventilation to survive acute respiratory distress syndrome.
The Link to Critical Care Interventions
The narrowing of the larynx is rarely a direct result of the SARS-CoV-2 virus itself, but rather a consequence of the life-saving measures employed in intensive care units. The insertion and prolonged presence of an endotracheal tube can cause pressure necrosis and mucosal injury to the delicate tissues of the larynx, and trachea.

According to recommendations from the Société française de phoniatrie et de laryngologie, patients subjected to prolonged intubation have shown a significant frequency of laryngotracheal complications. These include laryngeal immobility, inflammation, and edema of the vocal folds, which can progress to full laryngotracheal stenosis.
The process typically begins with localized inflammation at the site where the tube cuff presses against the airway wall. If this inflammation persists or leads to ischemia, the resulting healing process can produce dense fibrotic tissue, which gradually narrows the diameter of the airway.
Identifying Symptoms and Diagnosis
Laryngeal stenosis is often described as a complex and misunderstood
sequela because its symptoms may not appear immediately after a patient is extubated. The scarring process can take weeks or months to manifest, meaning patients may be discharged from the hospital before the airway begins to narrow significantly.
Common clinical indicators of this condition include:
- Stridor: A high-pitched, wheezing sound during inhalation, which is a hallmark of upper airway obstruction.
- Dyspnea: Increased shortness of breath, particularly during physical exertion, which may be mistaken for lingering lung damage.
- Dysphonia: Changes in voice quality or chronic hoarseness, especially if the stenosis affects the glottic region or the anterior commissure.
Diagnosis typically requires specialized endoscopic evaluation. Laryngoscopy allows physicians to visualize the exact location and severity of the narrowing, while computed tomography (CT) scans can help determine the length of the stenotic segment and the involvement of the surrounding cartilage.
Treatment and Long-term Management
The management of post-COVID laryngeal stenosis depends on the grade of the obstruction. For mild cases, clinicians may employ endoscopic dilation, where balloons are used to widen the airway under local or general anesthesia.
In more severe or recurrent cases, surgical intervention is necessary. This may involve a laryngotracheal resection, where the narrowed segment of the airway is removed and the healthy ends are sewn back together. Such procedures require a high level of surgical expertise and often necessitate a period of postoperative stenting or tracheostomy to ensure the airway remains open during healing.
Recovery often involves a multidisciplinary approach, combining surgical correction with speech and language therapy to restore vocal function and ensure the patient can breathe efficiently without respiratory distress.
Clinical Outlook
As the medical community continues to track “long COVID” and post-acute sequelae of the pandemic, the identification of laryngeal stenosis serves as a reminder of the long-term impact of critical care. While the immediate crisis of the pandemic has passed, the physical legacy of prolonged intubation continues to require specialized attention from otorhinolaryngologists and respiratory therapists.
