Cancer Cachexia: Mechanisms and Targeted Therapies
- For decades, cancer cachexia - the debilitating syndrome characterized by profound weight loss, muscle wasting, and loss of appetite - has been considered largely untreatable.
- Cancer cachexia affects an estimated 50-80% of cancer patients, significantly impacting quality of life and treatment outcomes. Its often more directly responsible for mortality than the cancer itself.
- The research pinpoints the HIF-2 pathway as a critical driver of the metabolic dysfunction characteristic of cachexia.
Cancer Cachexia: A New Path to Treatment
Table of Contents
For decades, cancer cachexia – the debilitating syndrome characterized by profound weight loss, muscle wasting, and loss of appetite – has been considered largely untreatable. But groundbreaking research published online January 2, 2026, in Nature Medicine, fundamentally shifts this perspective. Two independent studies have identified a key mechanism driving cachexia, a reliable biomarker for its presence, and a potential therapeutic strategy, all centered around the Hypoxia-Inducible Factor-2 (HIF-2) pathway.
Cancer cachexia affects an estimated 50-80% of cancer patients, significantly impacting quality of life and treatment outcomes. Its often more directly responsible for mortality than the cancer itself. Until now, management has largely focused on supportive care – nutritional supplementation and exercise – with limited success in reversing the underlying process.
The HIF-2 Pathway: A Central Role
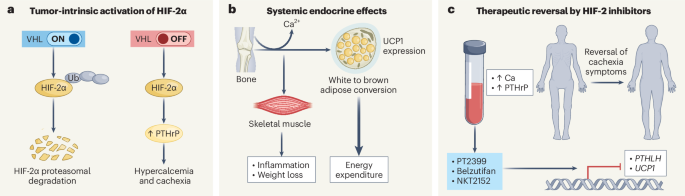
The research pinpoints the HIF-2 pathway as a critical driver of the metabolic dysfunction characteristic of cachexia. HIF-2, a protein activated in response to low oxygen levels, appears to be abnormally activated in cancer patients experiencing cachexia. This activation disrupts normal metabolic processes, leading to the breakdown of muscle tissue and the suppression of appetite.
Researchers discovered that blocking the HIF-2 pathway in preclinical models effectively reversed muscle wasting and improved overall metabolic health. This suggests that targeting HIF-2 could offer a novel therapeutic approach to combatting cachexia.
| Key Findings | implication |
|---|---|
| HIF-2 pathway activation | Drives muscle breakdown and metabolic dysfunction in cachexia. |
| HIF-2 inhibition | Reverses muscle wasting and improves metabolic health in preclinical models. |
| Identified Biomarker | Provides a means for early detection and monitoring of cachexia progression. |
A New Biomarker for Early Detection
Alongside the mechanistic insights, the studies also identified a specific biomarker associated with HIF-2 activation. While the exact nature of this biomarker hasn’t been publicly disclosed, its identification is crucial. Early detection of cachexia is vital, as interventions are likely to be most effective when initiated before notable muscle loss occurs. This biomarker will allow clinicians to identify patients at risk and monitor the effectiveness of potential treatments.
Therapeutic Strategies on the Horizon
The findings pave the way for the progress of targeted therapies aimed at inhibiting the HIF-2 pathway. Several pharmaceutical companies are already exploring HIF-2 inhibitors for other conditions,such as kidney cancer. Repurposing thes existing compounds, or developing new ones specifically for cachexia, could accelerate the availability of effective treatments.
These studies represent a paradigm shift in our understanding of cancer cachexia. For the first time, we have a clear therapeutic target and a potential strategy to reverse this devastating syndrome.
<
