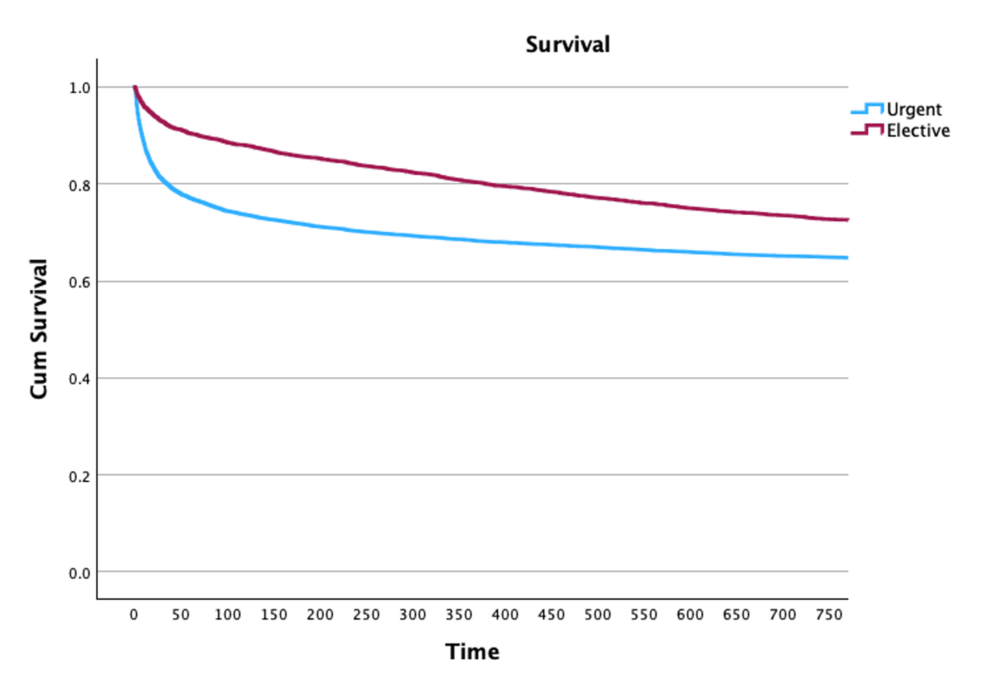
Elective vs. Urgent Surgery: ICU Outcomes Compared
- The intensity of care required following surgery varies significantly, and a new study highlights the importance of categorizing surgical procedures beyond the traditional ‘emergency’ versus ‘elective’ classifications.
- Traditionally, surgical cases have been broadly divided into emergency surgeries, performed to address life-threatening conditions, and elective surgeries, scheduled in advance for non-life-threatening issues.
- A retrospective review published in February 2017, and utilizing data from the American College of Surgeons National Surgery Quality Improvement Program (ACS NSQIP), examined over 173,000 general surgery...
The intensity of care required following surgery varies significantly, and a new study highlights the importance of categorizing surgical procedures beyond the traditional ‘emergency’ versus ‘elective’ classifications. Researchers are finding that a third category – ‘urgent’ surgery – carries its own distinct risk profile, impacting intensive care unit (ICU) utilization and patient outcomes.
Traditionally, surgical cases have been broadly divided into emergency surgeries, performed to address life-threatening conditions, and elective surgeries, scheduled in advance for non-life-threatening issues. However, a growing number of surgeries fall into a gray area – those that are not immediately life-threatening like emergencies, but also cannot be reasonably delayed without risking patient health. These are classified as ‘urgent’ surgeries.
A retrospective review published in , and utilizing data from the American College of Surgeons National Surgery Quality Improvement Program (ACS NSQIP), examined over 173,000 general surgery cases performed between , and , at 435 hospitals nationwide. The analysis revealed that approximately 12% of these procedures were categorized as urgent. The study found that patients undergoing urgent surgery faced a significantly higher risk of complications and mortality compared to those undergoing elective procedures, though the risk was somewhat lower than that seen in emergency surgeries.
Specifically, when controlling for pre-existing risk factors assessed by the ACS NSQIP, the odds ratio for experiencing any complication was 1.38 for urgent surgeries compared to elective surgeries (95% Confidence Interval: 1.30-1.45, P < .001). The odds ratio for mortality was even more pronounced, at 2.32 for urgent surgeries versus elective surgeries (95% Confidence Interval: 2.00-2.68, P < .001). Emergency surgeries also showed elevated risk, with complication and mortality odds ratios of 1.65 (95% CI, 1.55-1.76, P < .001) and 2.91 (95% CI, 2.48-3.41, P < .001) respectively, when compared to elective procedures.
These findings underscore the need for more nuanced risk stratification in surgical patients. Simply categorizing a surgery as ‘nonelective’ isn’t sufficient, as it doesn’t capture the spectrum of urgency. Recognizing ‘urgent’ surgery as a distinct category allows for more accurate prediction of potential complications and mortality, potentially leading to improved resource allocation and patient care.
Another study, published in , assessed surgical outcomes following emergency abdominal exploration. This research indicated that patients undergoing emergency abdominal exploration (EAE) due to complications from major elective surgery generally tolerated the procedure relatively well compared to those undergoing EAE for primary emergencies. This suggests that the underlying health status of the patient and the reason for the emergency procedure play a significant role in determining outcomes.
The implications of these findings extend to intensive care unit (ICU) management. A study examining ICU utilization after elective surgery found that patients requiring unplanned admission from the ward after elective surgery had a higher severity of illness compared to those admitted directly from the operating room. While this study didn’t specifically focus on urgent surgeries, it highlights the importance of identifying patients at risk for post-operative complications and potentially requiring higher levels of care.
The research suggests that a more precise understanding of surgical urgency is crucial for optimizing patient care. By accurately identifying and categorizing urgent surgeries, healthcare providers can better anticipate potential risks, allocate resources effectively, and ultimately improve outcomes for patients undergoing these procedures. Further research is needed to refine the definition of ‘urgent’ surgery and to develop standardized metrics for risk stratification, ensuring that all patients receive the appropriate level of care.
It’s important to remember that these studies identify statistical trends and do not predict the outcome for any individual patient. Surgical risk is complex and depends on a multitude of factors, including the patient’s overall health, the specific procedure being performed, and the expertise of the surgical team. Patients should always discuss their individual risks and benefits with their surgeon before undergoing any surgical procedure.
