Frantz Tumor: Case Report of Mimicking Pancreatic Pseudocyst
- A rare pancreatic tumor, known as a solid pseudopapillary neoplasm (SPN) or “Frantz tumor,” can sometimes mimic more common pancreatic conditions, leading to diagnostic challenges.
- SPNs are unusual, accounting for only 1-2% of all pancreatic tumors.
- The Frantz tumor, first described by Frantz in 1959, is generally considered to be an indolent, or slow-growing, tumor.
A rare pancreatic tumor, known as a solid pseudopapillary neoplasm (SPN) or “Frantz tumor,” can sometimes mimic more common pancreatic conditions, leading to diagnostic challenges. This was highlighted in a recent case report detailing a patient whose tumor was initially suspected to be an infected pancreatic pseudocyst.
SPNs are unusual, accounting for only 1-2% of all pancreatic tumors. They are most frequently found in young women, though, as one recent case study demonstrates, they can occur in patients of varying ages. The exact cause of these tumors remains unclear.
Understanding Solid Pseudopapillary Neoplasms
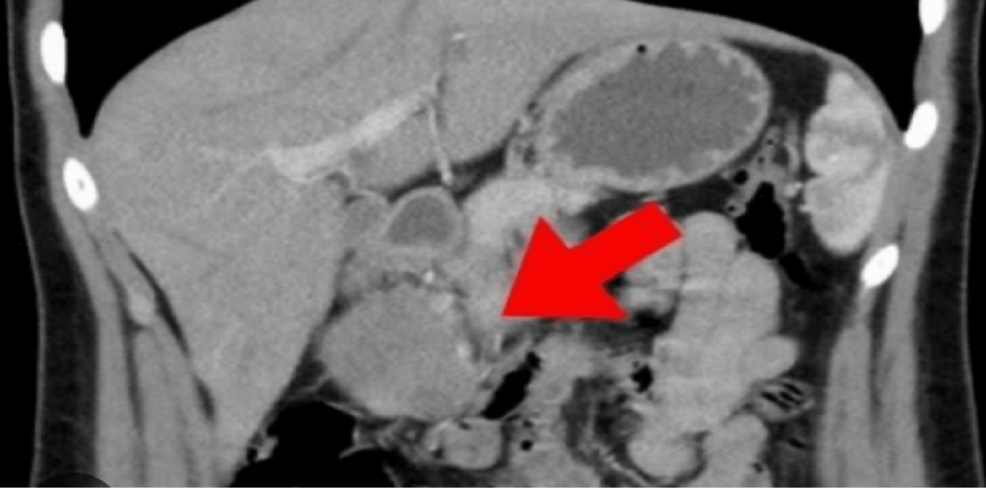
The Frantz tumor, first described by Frantz in 1959, is generally considered to be an indolent, or slow-growing, tumor. However, it can still present with significant symptoms, such as abdominal pain. The case report details a 60-year-old female patient who presented with occasional abdominal pain. Imaging studies, including positron emission tomography/computed tomography (PET/CT) and magnetic resonance imaging (MRI), revealed a mass in the tail of her pancreas.
Diagnosing SPNs can be complex. The imaging differential diagnosis can include other pancreatic cysts and tumors, such as complicated pancreatic pseudocysts, hydatid cysts, and mucinous cystic neoplasms. This complexity is underscored by the initial misdiagnosis in the reported case, where the tumor was initially suspected to be an infected pseudocyst.
Diagnosis and Treatment
Definitive diagnosis typically requires surgical removal of the tumor and subsequent pathological examination. In the case report, the patient underwent a distal pancreatectomy and splenectomy – surgical removal of the tail of the pancreas and the spleen. Pathology confirmed the diagnosis of SPN.
While SPNs are generally considered to have low malignant potential, some cases can exhibit locally aggressive behavior. Following surgery, the patient in the case report received four cycles of adjuvant chemotherapy with gemcitabine. A follow-up scan five months after the operation showed a suspicious cystic lesion, raising concerns about local recurrence. However, further examination revealed chronic indurative pancreatitis, areas with steatonecrosis, lipogranulomas, and fibrosis – indicating inflammation rather than a relapse of the tumor.
Key Considerations and Future Research
This case highlights the importance of considering SPN in the differential diagnosis of pancreatic masses, even in older patients. It also underscores the potential for post-operative inflammation to mimic tumor recurrence on imaging studies. Distinguishing between true recurrence and inflammatory changes can be challenging and may require further investigation.
The prognosis for patients with SPN is generally excellent after complete surgical resection. However, ongoing monitoring is crucial to detect any potential recurrence or complications. Further research is needed to better understand the histogenesis – the origin and development – of these tumors and to optimize treatment strategies.
According to research published in , SPNs have a general female predominance. However, the recent case demonstrates that the tumor can occur in both men and women, and at various ages. The tumor’s low malignant potential is a positive factor, but careful monitoring and appropriate surgical intervention remain critical for successful management.
The case report emphasizes that while SPNs are rare, they should be considered in the evaluation of pancreatic masses, particularly in young women. Accurate diagnosis and complete surgical resection are essential for achieving favorable outcomes. The potential for post-operative inflammatory changes to mimic recurrence also highlights the need for careful interpretation of follow-up imaging studies.
