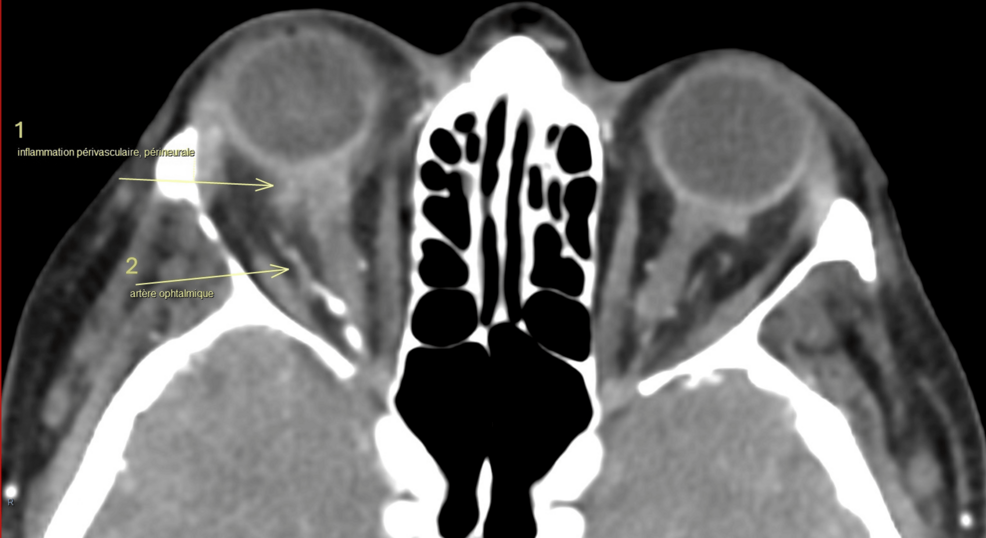
Giant Cell Arteritis: Cranial and Systemic Manifestations
- Giant cell arteritis (GCA) is a systemic vasculitis that primarily affects large and medium-sized arteries in individuals over the age of 50.
- Medical literature, including analysis published in Cureus and other clinical reviews, emphasizes that cranial and systemic manifestations of GCA are often two sides of the same coin.
- Cranial GCA typically involves the inflammation of the temporal arteries and other branches of the external carotid artery.
Giant cell arteritis (GCA) is a systemic vasculitis that primarily affects large and medium-sized arteries in individuals over the age of 50. While often recognized by its impact on the cranial arteries, the disease frequently manifests as a broader systemic condition, presenting a complex clinical spectrum that can involve both the head and the rest of the body.
Medical literature, including analysis published in Cureus and other clinical reviews, emphasizes that cranial and systemic manifestations of GCA are often two sides of the same coin
. In other words that while a patient may present with localized symptoms in the head, the underlying inflammatory process is systemic and can affect various large vessels throughout the body.
Cranial Manifestations and Risks
Cranial GCA typically involves the inflammation of the temporal arteries and other branches of the external carotid artery. The most critical risk associated with these manifestations is permanent vision loss, which occurs when the inflammation affects the ophthalmic artery or the posterior ciliary arteries, leading to anterior ischemic optic neuropathy.
Common cranial symptoms include:
- New-onset localized headaches, often centered around the temples.
- Scalp tenderness, which may be noticed when brushing hair or wearing glasses.
- Jaw claudication, described as pain or fatigue in the jaw muscles during chewing.
- Visual disturbances, including transient blurring or complete loss of vision.
Systemic and Large-Vessel Involvement
Beyond the cranial region, GCA can manifest as large-vessel vasculitis. This involves inflammation of the aorta and its major branches, such as the subclavian, axillary and brachial arteries. Systemic involvement can lead to a variety of non-specific symptoms that often precede or accompany the more localized cranial signs.
Many patients experience constitutional symptoms, including fever, night sweats, weight loss, and profound fatigue. A significant portion of GCA patients suffer from polymyalgia rheumatica (PMR), a condition characterized by stiffness and aching in the shoulders, and hips. While PMR can occur independently, its presence in an older adult often serves as a clinical red flag for the development of GCA.
Large-vessel involvement can also lead to more severe complications, such as aortic aneurysms or ischemia in the limbs, depending on which major arteries are affected by the inflammatory process.
Diagnostic Challenges and Approaches
Diagnosing GCA requires a high index of suspicion because the presentation varies significantly between patients. Traditionally, a temporal artery biopsy has been the gold standard for confirming a diagnosis of cranial GCA. However, this invasive procedure may not capture the inflammation if the disease is patchy or if the involvement is primarily in the large vessels rather than the cranial arteries.
To address these challenges, clinicians are increasingly utilizing imaging techniques. Positron Emission Tomography (PET) scans and Magnetic Resonance Angiography (MRA) allow physicians to visualize inflammation in the aorta and other large vessels, helping to identify systemic GCA in patients who may not exhibit classic cranial symptoms.
Management and Treatment Goals
The primary goal of GCA treatment is to reduce inflammation rapidly to prevent irreversible complications, particularly blindness. High-dose glucocorticoids remain the mainstay of therapy, often initiated immediately upon clinical suspicion even before biopsy results are available.
Because long-term steroid use carries significant risks—including osteoporosis, diabetes, and hypertension—physicians often introduce glucocorticoid-sparing agents. Recent clinical guidance highlights the use of tocilizumab, an interleukin-6 receptor inhibitor, which has emerged as an effective treatment for reducing the steroid burden while maintaining disease remission.
The dual nature of GCA—affecting both the cranial and systemic vasculature—underscores the necessity of a comprehensive diagnostic approach that looks beyond the temples to ensure all manifestations of the disease are managed.
