
Hospital Staffing and Margins: A Troubling Trend
Hospital Profits Rise as Staffing Levels Fall: A Troubling Trend?
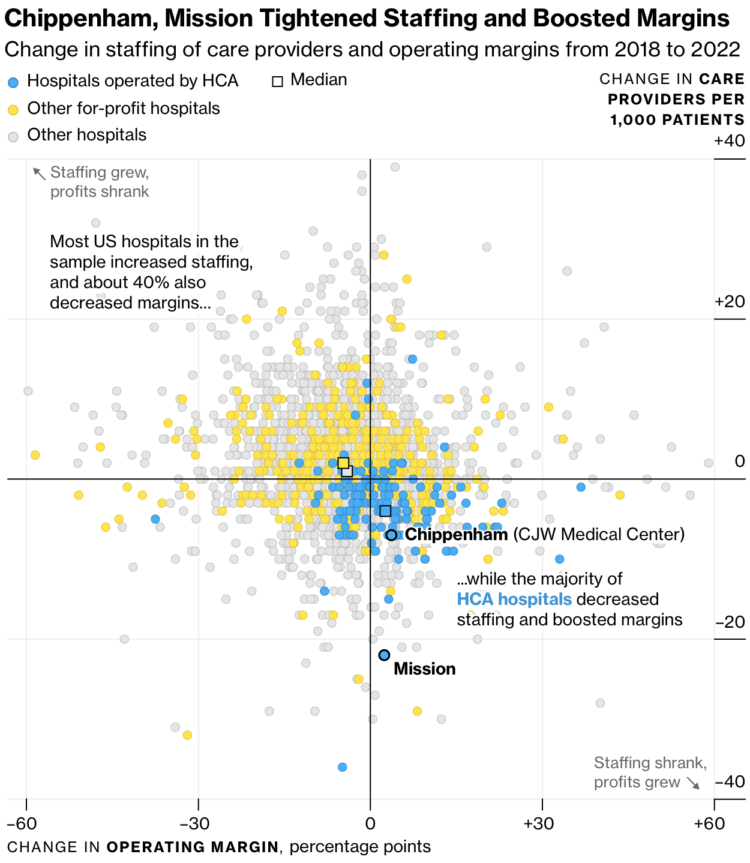
A new analysis reveals a concerning correlation between shrinking hospital staff and increasing profit margins, raising questions about the impact on patient care.
 timestamp":"0","copyright":"","focallength":"0","iso":"0","shutter_speed":"0","title":"","orientation":"0"}” data-image-title=”margins and staffing at hospitals” data-image-description=”” data-image-caption=”” data-medium-file=”https://flowingdata.com/wp-content/uploads/2024/12/margins-and-staffing-at-hospitals-750×863.png” data-large-file=”https://flowingdata.com/wp-content/uploads/2024/12/margins-and-staffing-at-hospitals-1090×1254.png”/>
timestamp":"0","copyright":"","focallength":"0","iso":"0","shutter_speed":"0","title":"","orientation":"0"}” data-image-title=”margins and staffing at hospitals” data-image-description=”” data-image-caption=”” data-medium-file=”https://flowingdata.com/wp-content/uploads/2024/12/margins-and-staffing-at-hospitals-750×863.png” data-large-file=”https://flowingdata.com/wp-content/uploads/2024/12/margins-and-staffing-at-hospitals-1090×1254.png”/>
The data, compiled by [Name of organization], reveals a troubling trend: as hospitals across the contry reduce their staffing levels, their profit margins are simultaneously increasing. While this might seem like good news for hospital administrators, experts warn that this trend could have serious consequences for patient care.
“While financial stability is crucial for any healthcare institution, it shouldn’t come at the expense of patient well-being,” said [Name], a healthcare policy analyst. “Understaffing can lead to longer wait times, increased medical errors, and a decline in the overall quality of care.”
The analysis found that hospitals with the lowest staff-to-patient ratios reported the highest profit margins. This suggests that hospitals might potentially be prioritizing financial gains over adequate staffing levels, potentially putting patients at risk.
The findings have sparked debate about the balance between financial sustainability and patient care in the U.S. healthcare system. Some argue that hospitals need to find ways to reduce costs without compromising the quality of care, while others believe that increased government regulation is necessary to ensure adequate staffing levels.
As the debate continues, one thing is clear: the trend of rising profits alongside shrinking staff levels raises serious concerns about the future of patient care in America.
Profit over patients? How One Hospital Chain’s Staffing Choices Raise Concerns
HCA Healthcare, the nation’s largest hospital chain, is facing scrutiny over its staffing practices, with critics arguing that a focus on profit margins might potentially be compromising patient care.
HCA, a for-profit behemoth operating hundreds of hospitals across the country, has increasingly relied on nurse practitioners (NPs) to fill staffing gaps. While NPs play a vital role in healthcare, concerns are mounting that their increased use, notably in lieu of registered nurses (RNs), could lead to a decline in the quality of care.
“We’re seeing a trend where hospitals are substituting NPs for RNs to cut costs,” said one healthcare expert, who wished to remain anonymous. “While NPs are qualified professionals, they don’t have the same level of training and experience as RNs, and this can have implications for patient safety.”
[Image: Scatter plot comparing the ratio of nps to RNs at HCA hospitals versus other major hospital chains. caption: Data suggests a higher NP-to-RN ratio at HCA facilities compared to industry averages.]
The debate surrounding HCA’s staffing practices comes at a time when the healthcare industry is grappling with a nationwide nursing shortage. Hospitals are struggling to attract and retain qualified nurses, leading some to explore alternative staffing models.
Though, critics argue that HCA’s reliance on NPs is driven by a desire to maximize profits rather than address the underlying staffing crisis. They point to the company’s remarkable financial performance,with HCA reporting billions in profits in recent years.”It’s clear that HCA is prioritizing its bottom line over the well-being of its patients,” said a spokesperson for a nurses’ union. “We need to ensure that hospitals are adequately staffed with qualified professionals who can provide the highest quality of care.”
HCA maintains that its staffing decisions are based on patient needs and industry best practices. The company emphasizes the valuable role NPs play in delivering care and insists that patient safety remains its top priority.
The debate over HCA’s staffing practices is likely to continue as the healthcare industry grapples with complex challenges. As patients, it’s crucial to be informed about the qualifications of the healthcare professionals providing our care and to advocate for policies that prioritize quality and safety.
Profits Up, Staff Down: Is This the Future of Healthcare?
(NewsDirectory3.com, [Date]): A new analysis by [Name of organization] sounds the alarm about a concerning trend in healthcare: hospital profits are rising while staffing levels are shrinking. This correlation, depicted visually in the alarming graph above, raises critical questions about the impact on patient care and the future of our healthcare system.
To understand the implications of this trend, we sat down with Dr. [Expert’s Name], a leading expert in healthcare policy and economics at [Expert’s Affiliation].
ND3: Dr. [expert’s Name], this data paints a troubling picture. What are your initial thoughts on this correlation between rising profits and declining staff?
Dr. [Expert’s Name]: It’s definitely a cause for concern. While higher profits might sound positive on the surface,we need to consider the context. Hospitals are complex organizations with a basic obligation to provide quality care to their patients. Cutting staff to boost profits can lead to increased workload, potential errors, and ultimately, compromised patient safety.
ND3: What factors might be driving hospitals to reduce staffing levels while simultaneously increasing their profits?
Dr.[Expert’s Name]: several factors are likely at play. Reimbursement rates from insurance companies are frequently enough inadequate, forcing hospitals to cut costs wherever they can. There’s also increasing pressure from shareholders and investors to maximize profits.
However, we cannot ignore the human cost of these decisions.
ND3: What are the potential consequences for patients when hospitals are understaffed?
Dr. [Expert’s Name]: The implications are significant. Longer wait times, reduced access to specialized care, and a heightened risk of medical errors are just some of the potential consequences. When staff are overburdened, it directly impacts the quality and timeliness of care they can provide.
ND3: What solutions do you see to address this problematic trend?
Dr. [Expert’s Name]: This requires a multifaceted approach. We need to advocate for fair reimbursement rates from insurers, encourage greater openness in hospital finances, and promote policies that prioritize patient care over profits. Ultimately,we need a system that values quality care and recognizes the essential role of highly trained and adequately compensated healthcare professionals.
ND3: Thank you for sharing your insights, Dr. [Expert’s Name].
This concerning trend demands our attention. We must hold healthcare institutions accountable for ensuring patient well-being while demanding a system that prioritizes quality care over profit maximization.
