HPV Vaccine Impact on Non-Cervical Cancers in HIV+ Patients
- new data presented at CROI 2025 highlights the crucial importance of human papillomavirus (HPV) vaccination in reducing the burden of non-cervical cancers in people living with HIV.
- While the impact of the relationship between HIV and HPV on the burden of cervical cancer is well-documented, less is known about non-cervical cancers related to human papillomavirus...
- Annually, 925,522 HPV-related cancers occur, with 77% of these cases in developing countries, resulting in 463,770 deaths.
HPV Vaccination: A Critical Tool for Reducing Cancer Burden in People Living with HIV
Table of Contents
- HPV Vaccination: A Critical Tool for Reducing Cancer Burden in People Living with HIV
- HPV Vaccination adn People Living with HIV: Key Questions Answered
- What is the link between HIV and HPV?
- Which cancers are related to HPV?
- What is the global impact of HPV-related cancers?
- What are the WHO’s goals for HPV vaccination?
- How does HPV prevalence and HIV affect cancer burden?
- What impact does increased vaccination coverage have?
- What are the key takeaways for HPV prevention in PLHIV?
- What are the current barriers to HPV prevention in developing countries?
- HPV and HIV: Key Statistics and Facts
new data presented at CROI 2025 highlights the crucial importance of human papillomavirus (HPV) vaccination in reducing the burden of non-cervical cancers in people living with HIV.
The Link Between HIV, HPV, and Cancer
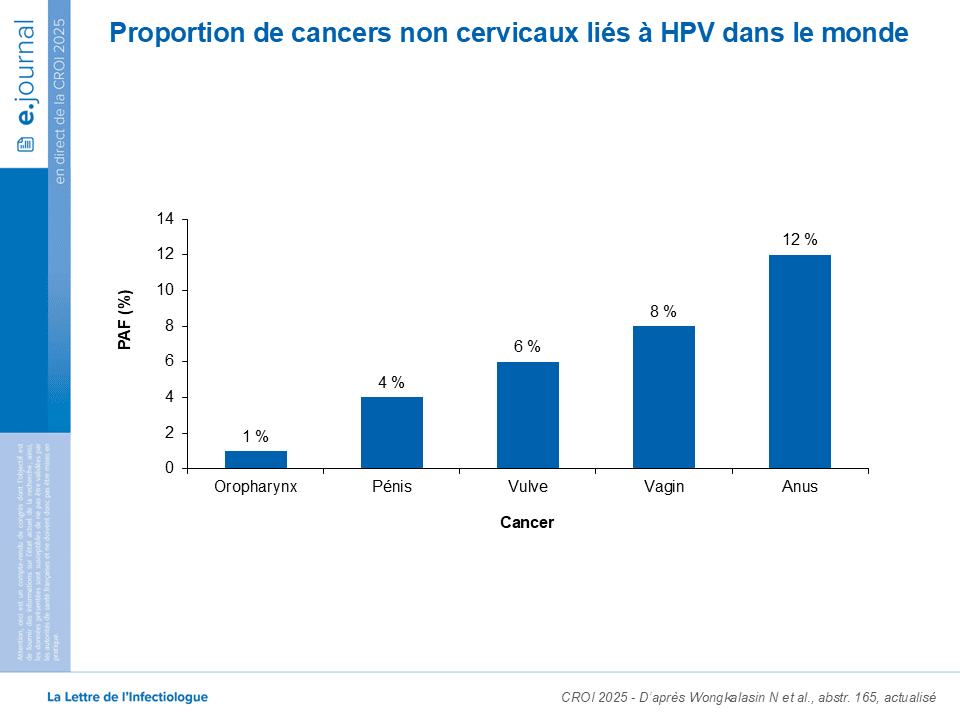
While the impact of the relationship between HIV and HPV on the burden of cervical cancer is well-documented, less is known about non-cervical cancers related to human papillomavirus (HPV), including cancers of the anus, oropharynx, vagina, vulva, and penis.
Annually, 925,522 HPV-related cancers occur, with 77% of these cases in developing countries, resulting in 463,770 deaths. The World Health Association (WHO) aims to vaccinate 90% of girls under 15 against HPV. However, global vaccination coverage remains low, at 21% for girls and 7% for boys. Coverage is particularly low in countries with a high prevalence of HIV. It’s critically important to note that HIV doubles the risk of HPV acquisition, and vice versa.
study Methodology and findings
Researchers sought to evaluate the burden of non-cervical cancers related to HPV in people living with HIV (PLHIV) and to model the potential impact of improved HPV vaccination coverage worldwide. They gathered epidemiological data on cancer incidence in 185 countries from the GLOBOCAN 2022 database. HIV prevalence data was obtained from UNAIDS 2022, which analyzes country-specific rates. The number of cancer cases was combined with the relative risks of developing each cancer and HIV prevalence data to generate a population attributable fraction, estimating the number of cancers “attributable” to HIV. they modeled the impact of improved vaccination coverage using point estimates of vaccine efficacy and country-specific HPV vaccination coverage levels provided by the WHO.
Geographical Variations in Cancer Burden
The study revealed notable geographical variations in the cancer burden. It was found that “29% of all non-cervical cancer cases related to HPV in Africa could be attributable to HIV, compared to 5% worldwide.”
Impact of Increased Vaccination Coverage
The researchers demonstrated that among the 10 countries with the highest number of cancers attributable to HIV, only two had vaccination coverage rates above 50%. Globally, their model shows that if non-gender-specific vaccination coverage increases to meet the 90% target set by the WHO, 6,854 cancer cases in PLHIV would be prevented, more than double the number currently avoided.
the Need for Further Research and Action
This analysis reinforces the consensus that PLHIV deserve special attention in HPV prevention. Further research on vaccine efficacy in PLHIV is needed to inform future analyses. New recommendations on the vaccination schedule and the number of doses could help to advance prevention efforts.
HPV Vaccination adn People Living with HIV: Key Questions Answered
Human papillomavirus (HPV) is a common virus linked to several types of cancer, especially in people living with HIV (PLHIV). Recent data presented at CROI 2025 emphasizes the importance of HPV vaccination in reducing the cancer burden in this population. This article answers crucial questions about HPV, HIV, vaccination, and cancer prevention.
What is the link between HIV and HPV?
HIV and HPV have a complex relationship. HIV weakens the immune system, making PLHIV more susceptible to persistent HPV infections and subsequent HPV-related diseases, including cancers. It is indeed also critical to note that HIV doubles the risk of HPV acquisition, and vice versa.
HPV is primarily known for causing cervical cancer. However, it’s also linked to several non-cervical cancers, including:
Anal cancer
Oropharyngeal cancer (cancers of the back of the throat, including the base of the tongue and tonsils)
Vaginal cancer
vulvar cancer
penile cancer
Globally, HPV-related cancers are a significant health concern:
Cases per Year: 925,522
Deaths per Year: 463,770
Impact in Developing Countries: 77% of cases occur in developing countries.
What are the WHO’s goals for HPV vaccination?
The World Health Institution (WHO) aims to achieve 90% HPV vaccination coverage for girls under 15 years old. However, current global vaccination rates are considerably lower:
Girls: 21%
Boys: 7%
How does HPV prevalence and HIV affect cancer burden?
The number of cancer cases was combined with the relative risks of developing each cancer and HIV prevalence data to generate a population attributable fraction, estimating the number of cancers “attributable” to HIV. A recent study revealed significant geographical variations: “29% of all non-cervical cancer cases related to HPV in africa could be attributable to HIV, compared to 5% worldwide.”
What impact does increased vaccination coverage have?
Increasing HPV vaccination coverage could dramatically reduce cancer cases in PLHIV.
Modeled Impact: If non-gender-specific vaccination coverage increases to meet the WHO’s 90% target, an estimated 6,854 cancer cases in PLHIV could be prevented globally.
What are the key takeaways for HPV prevention in PLHIV?
PLHIV require focused attention in HPV prevention strategies due to their heightened risk.
Further Research Needed: Additional studies are necessary to assess vaccine efficacy specifically in PLHIV.
* Optimizing Vaccination Schedules: New recommendations regarding vaccination schedules and the number of doses could enhance prevention efforts.
What are the current barriers to HPV prevention in developing countries?
HPV vaccination and cervical cancer screening availability is extremely limited in developing settings, although efforts to scale up screening are ongoing in Zambia .
HPV and HIV: Key Statistics and Facts
| Fact | Statistic/Finding |
| ——————————————- | ——————————————————————————————————————————————– |
| Global HPV-related cancer cases annually | 925,522 |
| Global HPV-related cancer deaths annually | 463,770 |
| Proportion of cases in developing countries | 77% |
| WHO vaccination target (girls under 15) | 90% |
| Current global vaccination coverage (girls) | 21% |
| Increased Prevention | Globally, their model shows that if non-gender-specific vaccination coverage increases to meet the 90% target set by the WHO, 6,854 cancer cases in PLHIV would be prevented, more than double the number currently avoided. |
