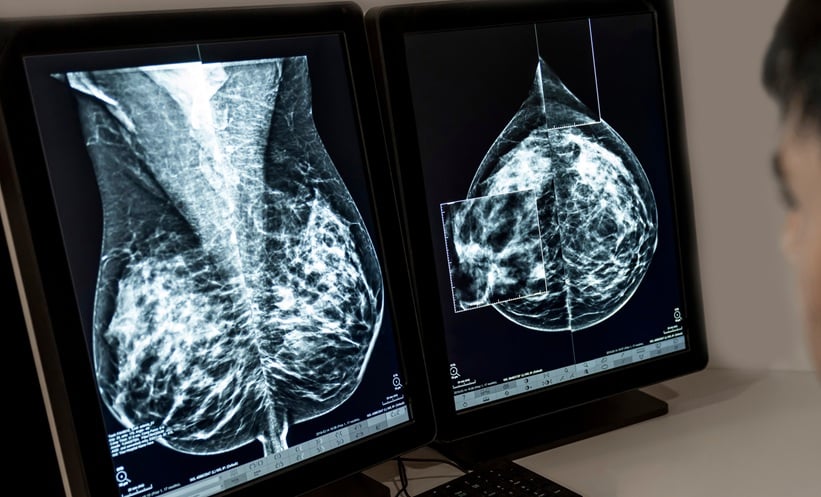
Mammography & Breast Cancer Surveillance: Lowering Mortality Risk (2026 Review)
- Annual mammographic surveillance remains a crucial component of post-treatment care for women with a history of breast cancer, significantly lowering mortality risk, according to a February 9, 2026...
- The analysis, which assessed studies evaluating mammography, ultrasonography, magnetic resonance imaging (MRI), and digital breast tomosynthesis, found that mammographic surveillance was linked to a 50% reduction in mortality...
- Breast cancer is the most commonly diagnosed cancer in women, and the number of survivors is steadily increasing globally, necessitating effective post-treatment surveillance strategies.
Annual mammographic surveillance remains a crucial component of post-treatment care for women with a history of breast cancer, significantly lowering mortality risk, according to a systematic review and meta-analysis. However, the accuracy of these screenings is often reduced in survivors compared to those undergoing initial breast cancer screening.
The analysis, which assessed studies evaluating mammography, ultrasonography, magnetic resonance imaging (MRI), and digital breast tomosynthesis, found that mammographic surveillance was linked to a 50% reduction in mortality risk. This underscores its continued importance despite inherent challenges in interpreting images of those who have undergone treatment.
The Challenges of Post-Treatment Imaging
Breast cancer is the most commonly diagnosed cancer in women, and the number of survivors is steadily increasing globally, necessitating effective post-treatment surveillance strategies. While mammography remains the cornerstone of this surveillance, its diagnostic accuracy is demonstrably lower in survivors than in women undergoing routine screening. This difference stems from several factors, including interval cancers – cancers that develop between screenings – and the presence of scar tissue and architectural distortion resulting from surgery and radiation therapy.
Breast-conserving therapy, which aims to remove cancerous tissue while preserving as much of the breast as possible, often leads to post-surgical and radiation-induced changes that can obscure the detection of subtle lesions. These changes can make it more difficult to differentiate between benign alterations and recurrent cancer.
Diagnostic Accuracy of Different Imaging Modalities
The meta-analysis examined the pooled sensitivity, specificity, and overall accuracy of mammographic surveillance. Results indicated a sensitivity of 81%, a specificity of 71%, and an overall accuracy of 76%. While these figures are lower than the 92% accuracy often cited for initial screening, they still demonstrate a significant benefit in terms of mortality reduction.
Notably, MRI demonstrated superior sensitivity (91%) and specificity (82%) compared to both mammography and ultrasonography. This suggests that adjunct imaging modalities, particularly MRI, can play a valuable role in enhancing early detection in breast cancer survivors, especially in cases where mammography is inconclusive or limited by post-treatment changes.
Study Methodology and Limitations
The systematic review and meta-analysis included eighteen studies that met the eligibility criteria, with eight contributing to the meta-analysis itself (three for diagnostic accuracy and five for mortality). Researchers conducted a comprehensive search of Medline, Cochrane Central Register of Controlled Trials, and Scopus databases to identify relevant studies. Data was synthesized using a random-effects model to account for variability between studies.
However, the researchers acknowledged several limitations. Significant heterogeneity was observed across studies, potentially stemming from variations in surveillance protocols, imaging frequency, and definitions of outcomes. Differences in mortality endpoints – some studies focused on breast cancer-specific mortality while others considered all-cause mortality – also contributed to this heterogeneity. The majority of included studies were conducted in high-income countries, limiting the generalizability of the findings to other populations.
Implications for Clinical Practice
The findings reinforce the importance of continued mammographic surveillance in post-treatment care, even acknowledging its limitations in this specific population. The lower diagnostic accuracy observed in survivors, compared to the general screening population, highlights the need for careful interpretation of imaging results and consideration of adjunct imaging modalities when appropriate.
Standardized surveillance protocols are crucial to improve post-treatment monitoring and optimize patient outcomes. These protocols should consider individual risk factors, treatment history, and imaging characteristics to tailor surveillance strategies to each patient’s specific needs.
Researchers also suggest that the integration of artificial intelligence (AI)-driven image processing in mammographic surveillance may further improve sensitivity and specificity. AI algorithms have the potential to identify subtle patterns and anomalies that might be missed by human observers, leading to earlier and more accurate detection of recurrence or second primary cancers.
While mammography isn’t a perfect test in this setting, the evidence clearly demonstrates its value in detecting recurrences and second primary breast cancers, ultimately improving survival rates. Continued research and refinement of surveillance strategies are essential to provide the best possible care for women with a history of breast cancer.
Reference
Icanervilia A V et al. Radiology surveillance for breast cancer survivors: a systematic review and meta-analysis. Asian Pac J Cancer Prev. ;27(2):433-442.
