
Medicaid for Seniors: 5 Key Facts (50+)
Proposed Medicaid Changes Could Impact Older Adults’ Coverage
Upcoming changes to Medicaid, considered as part of budget reconciliation, may disproportionately affect older adults, perhaps reducing coverage and access to long-term care. These changes include stricter enrollment requirements and adjustments to eligibility criteria.
Medicaid spending per person is significantly higher for those requiring long-term care services (LTSS). Spending for enrollees using long-term care was eight times greater than average Medicaid spending for enrollees who did not use any long-term care.

A critically important majority, 92%, of Medicaid enrollees ages 50 and older are enrolled through pathways that could be affected by reconciliation provisions, making it harder to enroll in and maintain Medicaid. This includes 27% through the Affordable Care Act (ACA) expansion pathway and 65% through pathways specifically for older adults and people with disabilities.
proposed spending cuts in reconciliation bills, including those in the House, stem from provisions affecting states that adopted the ACA Medicaid expansion. These cuts could total $427 billion over 10 years. Enrollment reductions are expected due to work requirements and more frequent eligibility redeterminations.
Further spending cuts, amounting to $167 billion, would result from delaying the implementation of rules streamlining Medicaid enrollment and renewal processes until 2035. These rules were expected to increase enrollment among those ages 65 and older or those with disabilities. The Congressional Budget Office (CBO) estimates that eliminating these rules would reduce Medicaid enrollment by 2.3 million in 2034, including 1.3 million dual-eligible individuals (those also on Medicare).

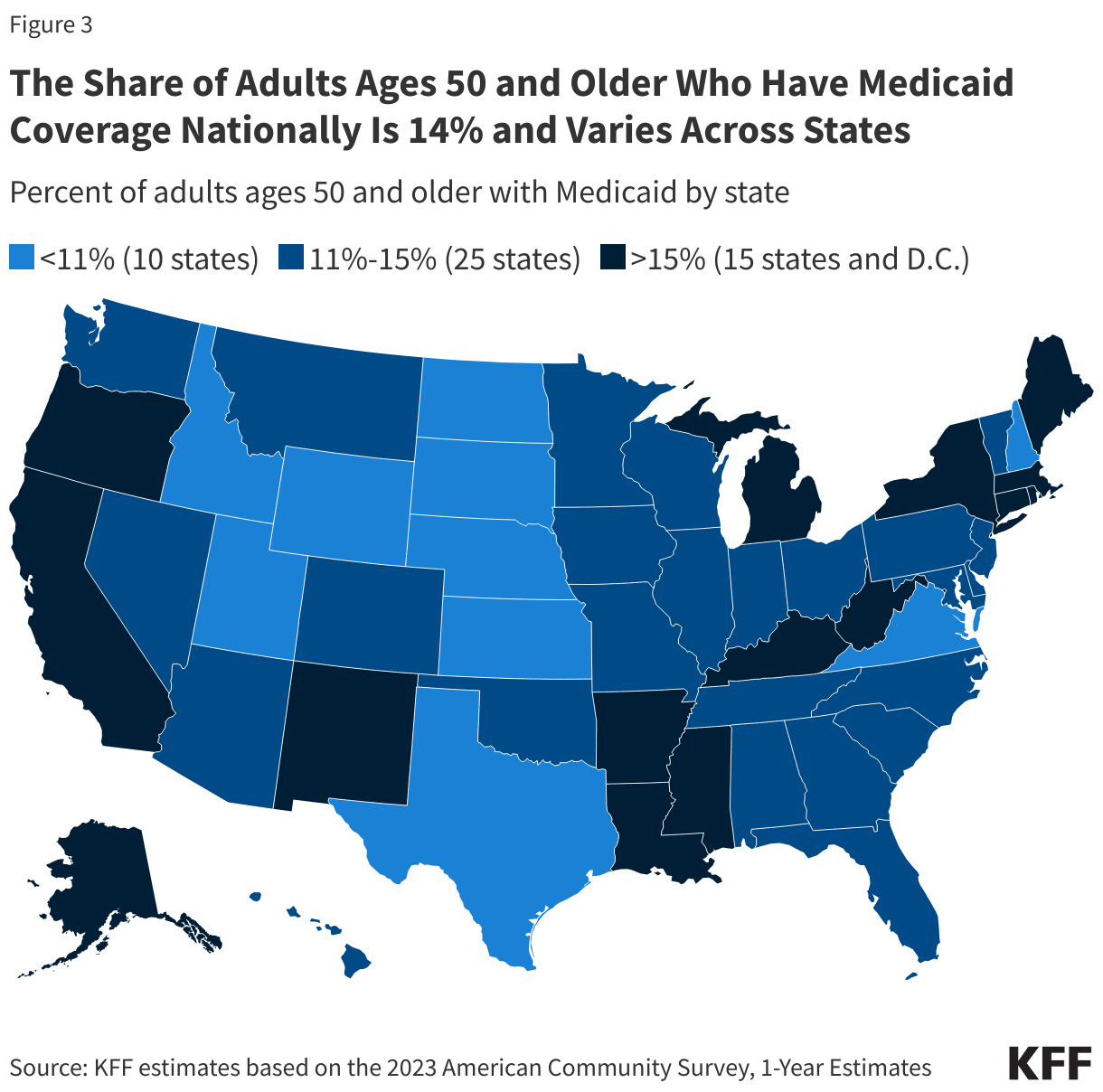
Nationally, 14% of adults ages 50 and older have Medicaid coverage, but this varies by state. States that expanded Medicaid under the ACA tend to have higher coverage rates (15%) compared to non-expansion states (12%). Higher Medicaid coverage rates are also observed in states with lower average incomes and fewer employer-sponsored health insurance options.
Most older adults on Medicaid are either working or face significant barriers to employment. Among adults ages 50 to 64 with medicaid who do not receive Social Security disability benefits,Supplemental Security Income (SSI),or Social Security Disability Insurance (SSDI),37% work full-time and 15% work part-time. Others report not working due to caregiving (9%), illness or disability (20%), or school attendance (1%).
A CBO report found that Medicaid work requirements are unlikely to increase employment rates but would likely result in loss of Medicaid coverage.Even with exemptions for caregiving and illness, reporting requirements increase the risk of losing coverage. In Arkansas, about 70% of those subject to work requirements lost coverage due to failure to report work status or document eligibility for an exemption.

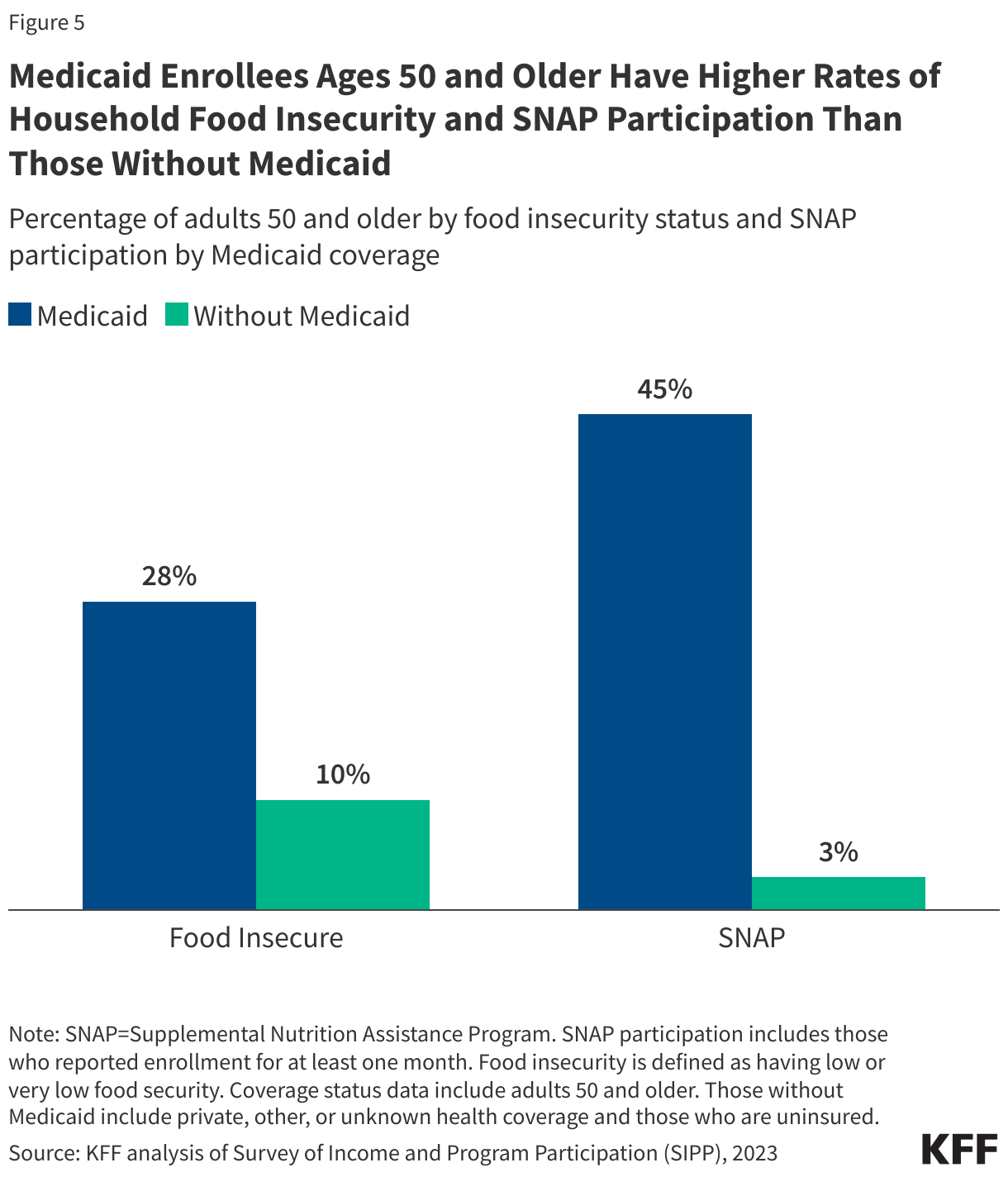
Proposed changes in reconciliation bills could also affect Supplemental Nutrition Assistance Program (SNAP) benefits, exacerbating financial challenges for older Medicaid enrollees. These enrollees already experience higher rates of household food insecurity compared to those without Medicaid. About 28% of Medicaid enrollees ages 50 and older live in households with food insecurity, compared to 10% of those not enrolled in Medicaid.
Nearly half (45%) of Medicaid enrollees ages 50 or older are enrolled in SNAP for at least one month, compared to 3% of their counterparts who are not enrolled in Medicaid. Loss of Medicaid coverage may also increase barriers to SNAP enrollment, as many states use medicaid enrollment to determine eligibility for other public benefit programs.
What’s next
The potential changes to Medicaid eligibility and enrollment processes will continue to be debated, with significant implications for older adults’ access to healthcare and nutrition assistance. Monitoring the outcomes of legislative actions and their effects on vulnerable populations remains crucial.
