Multiple Sclerosis: Understanding Its Two Different Forms
- Multiple sclerosis (MS) is a neurological condition characterized by nerve damage, though the specific pattern of that damage is unique to every individual.
- According to reporting from WebMD, the most common form of the disease is relapsing-remitting multiple sclerosis (RRMS), which affects approximately 85% of people with the condition.
- Individuals with RRMS typically encounter the first signs of the disease during their early 20s.
Multiple sclerosis (MS) is a neurological condition characterized by nerve damage, though the specific pattern of that damage is unique to every individual. Medical professionals categorize the disease into different types and progressive stages to help predict the potential severity of the illness and determine the most effective treatment options.
According to reporting from WebMD, the most common form of the disease is relapsing-remitting multiple sclerosis (RRMS), which affects approximately 85% of people with the condition.
Relapsing-Remitting Multiple Sclerosis
Individuals with RRMS typically encounter the first signs of the disease during their early 20s. This form of MS is defined by a cycle of attacks, known as relapses, which are followed by periods of recovery called remissions.
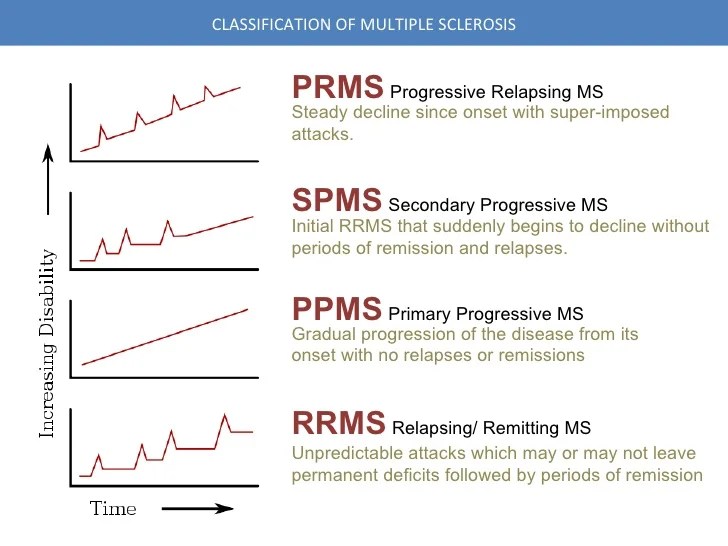
These remissions can last for weeks, months, or years. The nature of the disease varies significantly between patients, specifically regarding which nerves are affected, the severity of the attacks, the level of recovery achieved, and the duration of time between relapses.
Secondary Progressive Multiple Sclerosis
Many individuals who begin with RRMS eventually transition into a secondary progressive phase of the disease. In secondary progressive multiple sclerosis (SPMS), symptoms begin a steady decline without the distinct relapses or remissions seen in the earlier stage.
WebMD reports that this shift typically occurs between 10 and 20 years after the initial RRMS diagnosis. While the exact cause of this transition is not fully understood, research has identified specific factors that influence the timing:
- Patients who are older at the time of their initial diagnosis generally experience a shorter window before the disease becomes secondary progressive.
- Individuals who do not fully recover from their initial relapses tend to move into the secondary progressive phase more quickly than those who do achieve full recovery.
Physiologically, the process of nerve damage changes during this transformation. There is typically a decrease in inflammation and an increase in the slow decline of nerve function.
Early Clinical Pictures and Syndromes
Beyond the primary types of MS, the Belgian Charcot Foundation identifies other clinical pictures that are essential for classification and the adaptation of immunomodulatory treatments based on redefined 2013 criteria.
One such condition is radiologically isolated syndrome (RIS). This occurs when MS-suspected plaques are discovered accidentally during a brain MRI performed for unrelated reasons, such as head trauma, headaches, or a suspected pituitary tumour. People with RIS have no MS symptoms at the time of discovery.
While RIS does not require immediate treatment, follow-up MRI scans are advised for monitoring. The Belgian Charcot Foundation notes that one-third of patients with RIS will develop clinical MS within three years.
Another distinct clinical picture is clinically isolated syndrome (CIS). This involves individuals who experience a first inflammatory attack in the central nervous system with symptoms typical of MS. However, a definitive diagnosis of MS cannot be made in these cases because there is no evidence of dissemination in time or space.
Specifically, CIS is characterized by the absence of dual spatial and temporal dissemination, meaning there is only one detectable lesion and no combination of old inactive lesions with new active ones. The definitive diagnosis for these patients remains pending.
Clinical Significance of Classification
The distinction between these various forms of MS is critical for patient care. Accurate classification allows healthcare providers to better adapt immunomodulatory treatments to the specific needs of each patient.
Because the disease manifests differently—ranging from the episodic nature of RRMS to the steady progression of SPMS and primary progressive MS—the categories serve as a framework for managing the long-term trajectory of the illness.
