Optimizing Postoperative Recovery Beyond Opioid Pain Management
- Postoperative pain management is undergoing a significant shift as healthcare systems worldwide seek to balance effective recovery with the risks associated with opioid use.
- A systematic review and meta-analysis published in Updates in Surgery on April 20, 2026, examined the impact of opioid-sparing analgesia in minimally invasive colorectal surgeries.
- The findings align with broader trends in postoperative care, where short-term opioid use is increasingly scrutinized for its potential to delay recovery or contribute to longer-term dependency.
Postoperative pain management is undergoing a significant shift as healthcare systems worldwide seek to balance effective recovery with the risks associated with opioid use. Recent studies and clinical protocols highlight the growing adoption of opioid-sparing strategies in surgical recovery pathways, particularly within enhanced recovery after surgery (ERAS) programs. These approaches aim to reduce reliance on traditional opioid medications while maintaining patient comfort and accelerating functional recovery, especially in procedures like hip surgery where early mobility is critical to long-term outcomes.
Opioid Use and Early Functional Recovery
A systematic review and meta-analysis published in Updates in Surgery on April 20, 2026, examined the impact of opioid-sparing analgesia in minimally invasive colorectal surgeries. The study compared opioid-based and opioid-sparing perioperative pain management strategies across 21,216 patients, with 18.6% (1,840 patients) receiving opioid-sparing regimens. While postoperative pain levels at 24 and 48 hours showed no statistically significant difference between the two groups—measured using the visual analog scale (VAS)—opioid-sparing strategies led to a substantial reduction in postoperative opioid consumption. Patients in the opioid-sparing group required an average of 29.7 mg fewer morphine equivalents, a decrease of nearly 30% compared to those receiving traditional opioid-based analgesia.
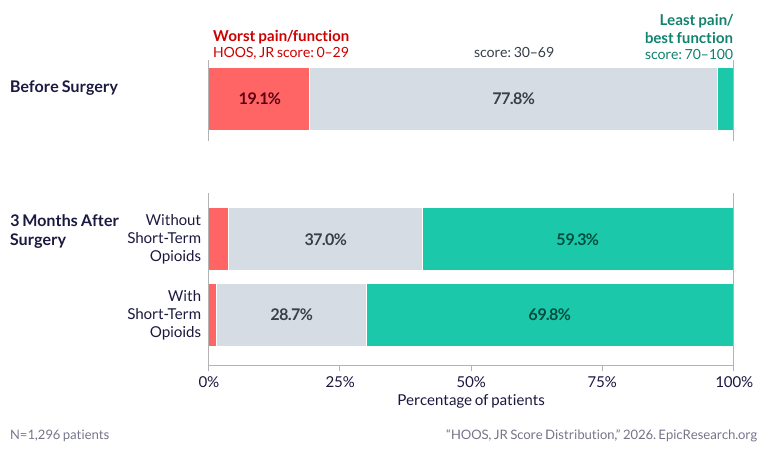
The findings align with broader trends in postoperative care, where short-term opioid use is increasingly scrutinized for its potential to delay recovery or contribute to longer-term dependency. A Google Alert discovery from April 28, 2026, highlighted research suggesting that limited, short-term opioid prescriptions may actually improve early functional recovery after hip surgery. This counterintuitive outcome is attributed to reduced opioid-related side effects, such as nausea, dizziness, and sedation, which can impede physical therapy and mobility in the critical days following surgery.
Enhanced Recovery Pathways and Multimodal Pain Management
Enhanced recovery pathways (ERPs) have become a cornerstone of modern perioperative care, standardizing protocols to minimize complications and accelerate patient discharge. A 2022 study published in the Journal of Pain Research, authored by researchers at Brigham and Women’s Hospital and Harvard Medical School, emphasized the role of multimodal pain management in ERPs. The study, led by Christopher K. Cheung and Richard D. Urman, outlined strategies to reduce opioid dependence by combining regional anesthesia, non-opioid analgesics, and non-pharmacological interventions such as physical therapy and patient education.
Multimodal analgesia typically includes the use of acetaminophen, nonsteroidal anti-inflammatory drugs (NSAIDs), and regional nerve blocks, which target specific pain pathways without the systemic side effects of opioids. For example, advances in regional nerve blocks for laparoscopic gynecological surgery—highlighted in a recent Frontiers publication—demonstrate how precision techniques can provide targeted pain relief while minimizing opioid exposure. These innovations are particularly relevant in surgeries where early mobilization is associated with reduced complications, such as deep vein thrombosis and pneumonia.
The shift toward opioid-sparing strategies is not without challenges. The Updates in Surgery meta-analysis found no significant differences in hospital length of stay or complication rates, including nausea, pruritus, postoperative ileus, readmission, or mortality, between opioid-sparing and opioid-based groups. However, the reduction in opioid consumption itself is a critical outcome, given the ongoing public health concerns surrounding opioid prescriptions. In the United States alone, postoperative opioid prescriptions have been linked to persistent use in up to 6% of opioid-naïve patients, according to prior research cited in the Journal of Pain Research study.
Nursing and Patient-Centered Approaches
Nurses play a pivotal role in implementing and optimizing postoperative pain management strategies. A 2025 paper in the MedSurg Nursing Journal underscored the importance of evidence-based nursing practices in assessing and tailoring pain control regimens. The study highlighted that effective pain management extends beyond medication, incorporating patient education, psychological support, and continuous monitoring to adjust treatments in real time. For instance, patients who understand the benefits of non-opioid alternatives may be more willing to tolerate mild discomfort in exchange for faster recovery and fewer side effects.
Patient perspectives are increasingly integrated into pain management protocols. A multi-level consensus study published in Nature in 2026 focused on optimizing the deprescribing of hospital-initiated opioids. The study brought together clinicians, researchers, and patients to develop guidelines that balance pain control with the risks of prolonged opioid use. Key recommendations included setting clear expectations for postoperative pain, providing alternative pain relief options, and establishing follow-up protocols to monitor for signs of dependency or inadequate pain control.
Economic and Operational Implications
The adoption of opioid-sparing strategies has significant economic implications for healthcare systems. Reduced opioid consumption can lower the risk of adverse events, such as respiratory depression and prolonged hospital stays, which are costly to manage. Shorter recovery times and fewer complications can improve patient throughput in surgical units, a critical factor in healthcare systems facing capacity constraints.

Hospitals and insurers are also responding to regulatory pressures and public demand for safer pain management practices. In the U.S., the Centers for Medicare & Medicaid Services (CMS) have introduced quality metrics that incentivize hospitals to reduce opioid-related adverse events. Similarly, the Joint Commission, which accredits healthcare organizations, has updated its pain management standards to emphasize non-opioid alternatives and patient-centered care plans.
From a business perspective, pharmaceutical companies are investing in the development of non-opioid analgesics and regional anesthesia technologies. For example, long-acting local anesthetics and nerve block devices are gaining traction as alternatives to systemic opioids. These innovations not only address clinical needs but also open new markets for medical device and drug manufacturers.
Future Directions and Challenges
Despite the progress, challenges remain in widespread adoption of opioid-sparing strategies. Variability in surgical practices, patient preferences, and institutional protocols can hinder standardization. Some patients may still require opioids for adequate pain control, particularly in complex or highly invasive procedures. The Updates in Surgery meta-analysis noted that while opioid-sparing strategies are effective in minimally invasive colorectal surgeries, their applicability to other surgical specialties requires further study.
Future research is likely to focus on personalized pain management, leveraging data analytics and artificial intelligence to predict individual patient responses to different analgesic regimens. For example, machine learning models could identify patients at higher risk for prolonged opioid use, allowing clinicians to tailor pain management plans preemptively. Similarly, advancements in regional anesthesia, such as ultrasound-guided nerve blocks, are expected to improve precision and reduce complications.
As healthcare systems continue to refine postoperative pain management, the integration of opioid-sparing strategies into ERPs represents a critical step toward safer, more effective recovery pathways. The balance between pain control and opioid minimization is not merely a clinical challenge but a business imperative, with implications for patient outcomes, healthcare costs, and regulatory compliance. The shift is already underway, driven by evidence, innovation, and a growing recognition of the need to rethink traditional approaches to postoperative care.
