Scaling and Root Planing Impact on Inflammation in Periodontitis
Treatment with scaled root planing (SRP) led to a significant reduction in tumor necrosis factor-alpha (TNF-α) levels in both diabetic and non-diabetic patients (P < 0.001). Though, post-treatment TNF-α levels remained significantly higher in the diabetic group compared to the non-diabetic group (P < 0.001), suggesting a persistently elevated pro-inflammatory state in diabetic patients despite treatment.
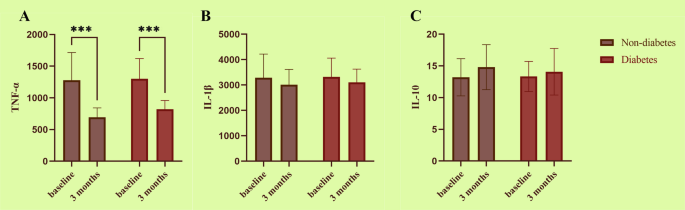
For interleukin-1 beta (IL-1β), levels in the non-diabetic group decreased from 3289.03 ± 929.39 pg/ml to 3012.45 ± 602.90 pg/ml, a reduction of 276.58 ± 1137.80 pg/ml. In the diabetic group, IL-1β declined from 3318.24 ± 741.78 pg/ml to 3101.50 ± 526.78 pg/ml (Δ = 216.74 ± 960.97 pg/ml). No statistically significant difference in the magnitude of reduction was found between groups (P = 0.805), and as shown in Fig. 3B, neither group exhibited a statistically significant within-group change in IL-1β following treatment.
Regarding the anti-inflammatory cytokine IL-10, post-treatment increases were observed in both groups. In the non-diabetic group, IL-10 levels increased from 13.21 ± 2.94 pg/ml to 14.81 ± 3.55 pg/ml (Δ = +1.60 ± 4.83 pg/ml), while in the diabetic group, levels rose from 13.33 ± 2.37 pg/ml to 14.08 ± 3.68 pg/ml (Δ = +0.75 ± 4.35 pg/ml). As shown in Fig. 3C, the increase in IL-10 was more pronounced in the non-diabetic group, although the between-group difference was not statistically significant (P = 0.422). Similarly, the absolute post-treatment IL-10 levels were slightly higher in the non-diabetic group (14.81 ± 3.55 pg/ml) than in the diabetic group (14.08 ± 3.68 pg/ml), but this difference also did not reach statistical significance (P = 0.384).
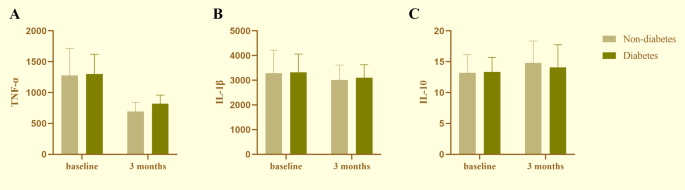
Figure 4 compares the changes in inflammatory cytokine levels between groups at baseline and three months post-treatment.although baseline values were similar, the non-diabetic group exhibited a more considerable decrease in TNF-α and a more noticeable increase in IL-10 following treatment. These findings suggest that non-diabetic individuals may have a more favorable inflammatory response to SRP.