TPS Program Changes and Their Impact on Healthcare Access
- Changes to Temporary Protected Status (TPS) designations by the Trump administration are creating significant risks for the health and healthcare access of thousands of noncitizens, according to an...
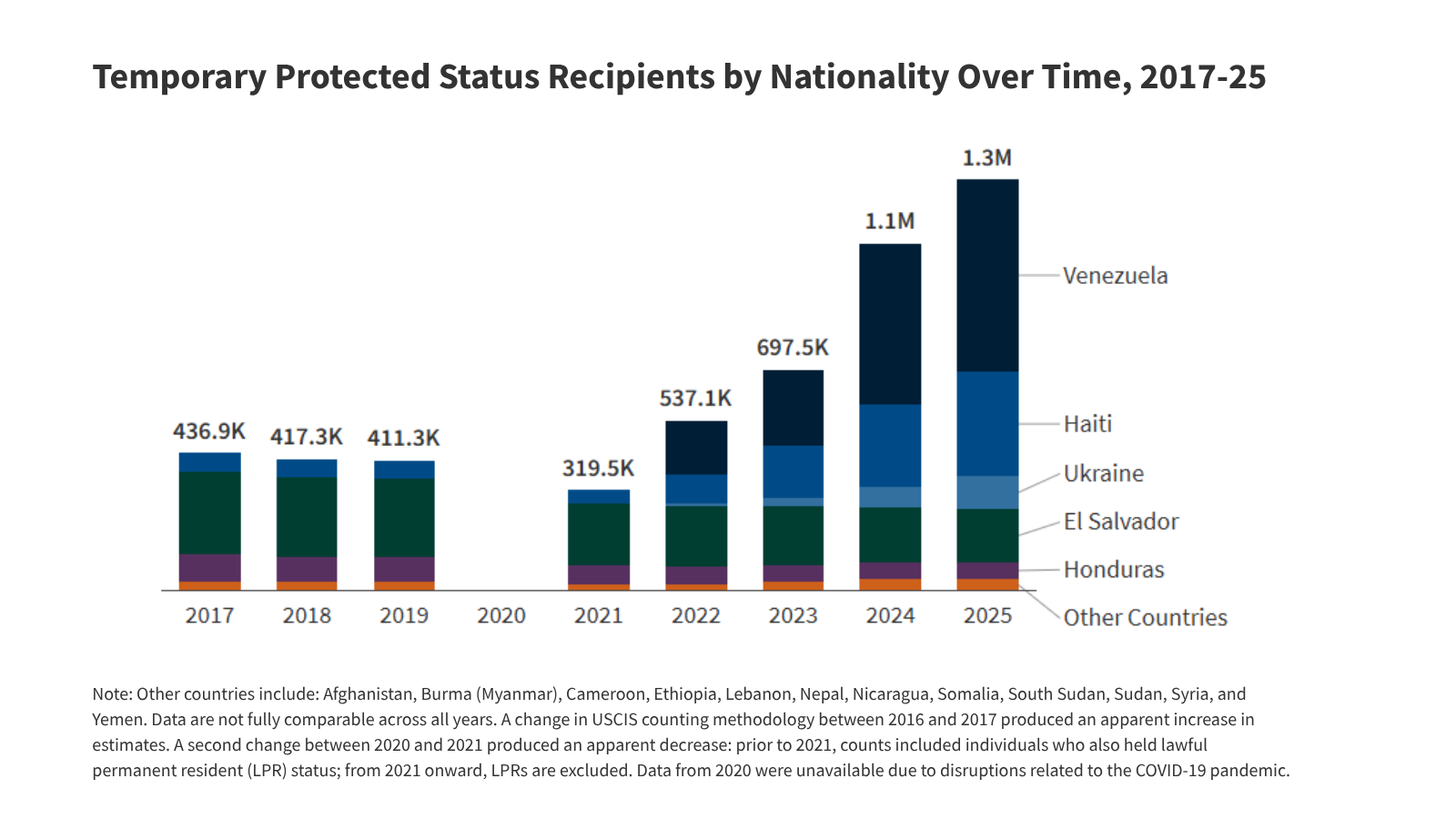
- TPS is a temporary status granted to nationals of countries experiencing ongoing armed conflict, environmental disasters, or other extraordinary and temporary conditions.
- The loss of this status can trigger a cascade of health-related challenges, primarily by removing the legal foundation required to maintain health insurance and access consistent medical care.
Changes to Temporary Protected Status (TPS) designations by the Trump administration are creating significant risks for the health and healthcare access of thousands of noncitizens, according to an analysis by the Kaiser Family Foundation (KFF).
TPS is a temporary status granted to nationals of countries experiencing ongoing armed conflict, environmental disasters, or other extraordinary and temporary conditions. This status provides individuals with protection from removal and authorization to work legally in the United States.
The loss of this status can trigger a cascade of health-related challenges, primarily by removing the legal foundation required to maintain health insurance and access consistent medical care.
Impacts on Health Insurance Coverage
A primary consequence of the termination of TPS is the loss of employment authorization. Because many TPS holders rely on employer-sponsored health insurance, the loss of a legal right to work often leads directly to a loss of medical coverage.
Without insurance, individuals are more likely to delay preventive screenings and necessary treatments for chronic conditions. This shift often pushes patients toward emergency departments for care that could have been managed more effectively and less expensively in a primary care setting.
the loss of TPS can make individuals ineligible for various state-funded health programs, further narrowing the available options for those who cannot afford private insurance.
Barriers to Healthcare Access
Beyond the financial barriers of insurance loss, the threat of deportation creates a chilling effect
that deters individuals from seeking medical attention. Fear of immigration enforcement at or near healthcare facilities often leads patients to avoid clinics and hospitals entirely.
This avoidance is particularly acute for those managing high-risk conditions such as diabetes, hypertension, or infectious diseases, where interrupted treatment can lead to severe health complications or public health risks.
The KFF analysis notes that the psychological stress associated with the uncertainty of legal status contributes to a rise in mental health challenges, including severe anxiety and depression, which often go untreated due to the aforementioned barriers to care.
Strain on the Health Workforce
The implications of TPS changes extend beyond the patients to the healthcare system’s operational capacity. Many TPS holders are employed within the health workforce, filling critical roles that sustain the U.S. Medical infrastructure.

These individuals frequently work as:
- Certified Nursing Assistants (CNAs)
- Home health aides
- Licensed practical nurses
- Medical assistants
The removal of these workers from the labor market exacerbates existing staffing shortages, particularly in long-term care facilities and home-based care services. This loss of personnel can reduce the quality of care for elderly and disabled populations who rely on these essential workers.
Public Health Implications
From a public health perspective, the disruption of care for TPS populations can hinder broader health initiatives. Effective management of communicable diseases requires consistent monitoring and treatment, which is compromised when a significant population is forced into the shadows.
The KFF brief suggests that when populations lose the ability to access routine care, the overall burden on the public health system increases as preventable conditions evolve into acute crises.
Medical providers are increasingly tasked with navigating the legal complexities of treating undocumented patients, often facing uncertainty regarding the legality of providing specific types of care or the availability of funding for those services.
