
Worrying Alzheimer’s-Virus Link Discovered
Herpes Virus Link to Alzheimer’s Disease Gains Traction in Research
Table of Contents
- Herpes Virus Link to Alzheimer’s Disease Gains Traction in Research
- Herpes Virus Link to Alzheimer’s Disease: What You Need to Know
- What is teh connection between the herpes virus and Alzheimer’s disease?
- How does the herpes virus perhaps contribute to Alzheimer’s disease?
- What is the APOE-E4 gene, and why is it relevant?
- How does HSV-1 cause brain damage?
- Are there other viruses linked to Alzheimer’s disease?
- Can vaccination or antiviral medications help prevent Alzheimer’s?
- What are the potential future directions based on this research?
- Is Alzheimer’s disease solely caused by viral infections?
- Summary of Key Findings
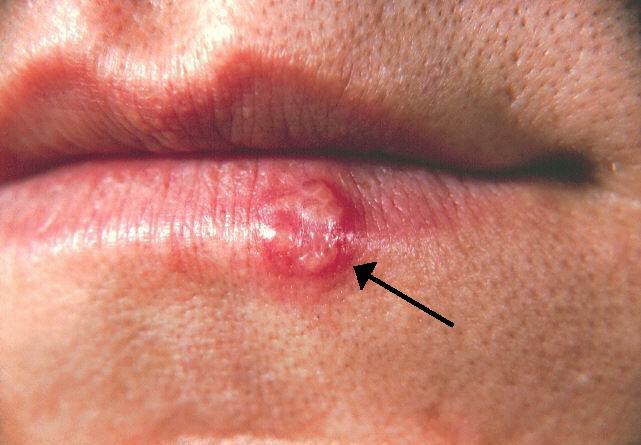
The herpes simplex virus type 1 (HSV-1), commonly associated with cold sores, may play a significant role in the progress of Alzheimer’s disease, according to emerging research.While typically contracted in childhood and remaining dormant within nerve cells, HSV-1 can reactivate due to factors like stress or illness. Scientists are now exploring its potential connection to neurodegenerative conditions.
More than three decades ago, a team led by Ruth Itzhaki, now an emeritus professor of molecular neurobiology at the University of manchester and a guest professor at the University of Oxford, identified the presence of the herpes virus in the brains of elderly individuals. this discovery challenged the prevailing belief that the brain was largely shielded from infection, thanks to the blood-brain barrier.
The research indicated that individuals carrying a specific variant of the APOE gene, known as APOE-E4, which is already linked to an increased risk of Alzheimer’s, were particularly vulnerable when HSV-1 was also present. this suggested a potential synergistic effect between the virus and genetic predisposition in the development of the disease.
Unraveling the Virus-Brain Damage Connection
Studies of brain cells infected with HSV-1 have revealed the production of abnormal proteins, including amyloid and tau, which are hallmarks of Alzheimer’s disease. Researchers hypothesize that the virus can remain dormant for extended periods before reactivating, particularly as the immune system weakens with age.
This reactivation within the brain can trigger inflammation and damage to brain cells. Over time, repeated instances of such damage could contribute to the onset of Alzheimer’s disease. Analyses have even detected viral DNA within the abnormal protein clusters found in the brains of Alzheimer’s patients.
Laboratory experiments have shown promising results. When infected brain cells were treated with antiviral drugs, the extent of damage was reduced. Moreover, large-scale studies have indicated a correlation between severe infections, including those caused by HSV-1, and a higher risk of dementia. These studies also suggest that patients treated with antiviral medications may have a lower risk of developing Alzheimer’s disease.
Exploring the Role of other Viruses
Research efforts have expanded to investigate other dormant viruses, such as the varicella-zoster virus, which causes chickenpox and shingles. A study analyzing medical records in the United Kingdom found that individuals vaccinated against shingles had a significantly lower risk of developing dementia.
Similar research from Stanford University corroborated these findings, reinforcing the idea that preventing certain infections could mitigate the risk of Alzheimer’s. These studies suggest that common viral infections may contribute to neurodegenerative diseases, and that preventative measures, such as vaccination, could be an effective strategy for reducing Alzheimer’s risk.
In laboratory settings, a 3D model of a brain infected with dormant HSV-1 was used to simulate the effects of other infections or head trauma. These events appeared to reactivate the virus,leading to damage similar to that observed in Alzheimer’s disease. Conversely, anti-inflammatory treatment prevented viral reactivation and subsequent brain lesions.
Implications and Future Directions
These findings suggest that HSV-1 could be a contributing factor in Alzheimer’s disease, particularly in individuals with genetic predispositions like the APOE-E4 gene. This opens avenues for new prevention strategies, including vaccines or antiviral treatments aimed at keeping the virus dormant. What initially appeared to be a simple connection between cold sores and memory loss has evolved into a promising area of research for understanding and possibly reducing the risk of this devastating disease.
While research continues, scientists emphasize that Alzheimer’s disease is highly likely multifactorial, and viral infection is just one piece of the puzzle.
Herpes Virus Link to Alzheimer’s Disease: What You Need to Know
What is teh connection between the herpes virus and Alzheimer’s disease?
Emerging research suggests a potential link between the herpes simplex virus type 1 (HSV-1), commonly associated with cold sores, and the development of Alzheimer’s disease. While HSV-1 typically lies dormant within nerve cells after initial infection, it can reactivate. Scientists are exploring how this reactivation might contribute to neurodegenerative conditions like alzheimer’s.
How does the herpes virus perhaps contribute to Alzheimer’s disease?
Several factors point toward a possible connection:
- Viral Presence in the Brain: Research, dating back more than three decades, has identified the presence of the herpes virus in the brains of elderly individuals.
- Synergistic Effect with Genetic Predisposition: Individuals with a specific variant of the APOE gene, known as APOE-E4 (which increases the risk of Alzheimer’s), appear particularly vulnerable when HSV-1 is present.
- Brain Damage: Studies show that HSV-1 infection in brain cells leads to the production of abnormal proteins associated with Alzheimer’s (amyloid and tau).
- Reactivation and Inflammation: Reactivation of the virus within the brain can trigger inflammation and damage brain cells, particularly as the immune system weakens with age.
- Antiviral Treatment benefits: Laboratory experiments show that antiviral drugs can reduce brain damage in infected cells. Large-scale studies suggest a correlation between severe infections, including HSV-1, and a higher risk of dementia, and also a lower risk of alzheimer’s in patients treated with antiviral medications.
What is the APOE-E4 gene, and why is it relevant?
The APOE-E4 gene is a specific variant of the APOE gene. This gene is already known to increase the risk of developing Alzheimer’s disease. Research suggests that the presence of both the APOE-E4 gene and HSV-1 may create a synergistic effect,making individuals even more susceptible to the disease. According to the provided text, individuals carrying the APOE-E4 gene are ”particularly vulnerable” when HSV-1 is also present.
How does HSV-1 cause brain damage?
Research indicates that HSV-1 can cause brain damage through several mechanisms:
- Production of Abnormal Proteins: Infection with HSV-1 leads to the production of abnormal proteins, including amyloid and tau, which are hallmarks of Alzheimer’s disease.
- Inflammation: Reactivation of the virus triggers inflammation in the brain.
- Cellular Damage: Repeated instances of inflammation and viral activity can damage brain cells over time.
Are there other viruses linked to Alzheimer’s disease?
Yes, research is extending to other viruses.The varicella-zoster virus, which causes chickenpox and shingles, is also under inquiry. Studies have found that individuals vaccinated against shingles have a lower risk of developing dementia.
The provided text suggests that preventative measures, such as vaccination and antiviral medications, may play a role in reducing the risk of Alzheimer’s disease.
* Vaccination: Studies indicate that vaccination against shingles (caused by the varicella-zoster virus) may lower the risk of dementia.
* Antiviral Medications: Laboratory experiments and large-scale studies suggest that antiviral drugs, used to treat infections like HSV-1, may reduce the extent of brain damage and lower the risk of developing Alzheimer’s disease.
What are the potential future directions based on this research?
The findings open avenues for new prevention strategies. These include:
- Vaccines aimed at preventing initial HSV-1 infection.
- Antiviral treatments designed to keep the virus dormant, particularly in individuals with genetic risk factors.
No, research emphasizes that Alzheimer’s disease is highly likely multifactorial. Viral infection is just one piece of the complex puzzle, along with genetic predisposition, lifestyle and other health factors.
Summary of Key Findings
This table summarizes the key points about the link between HSV-1 and alzheimer’s disease:
| Aspect | Details |
|---|---|
| Virus Involved | Herpes Simplex virus type 1 (HSV-1) |
| Primary Association | Cold sores |
| Potential Link | Increased risk and progression of Alzheimer’s disease |
| Mechanism | Reactivation of HSV-1 in the brain, leading to inflammation, production of abnormal proteins, and cell damage. |
| Risk Factors | APOE-E4 gene |
| Potential Prevention | Vaccines, antiviral medications |
