Medicaid Home Care (HCBS) 2025: Changes & Benefits
Many older adults and people with disabilities require assistance with self-care such as bathing, dressing, and eating. Help with such services is known as “long-term care” and may be provided in institutional settings such as nursing facilities or in people’s homes and the community, including assisted living facilities. Four-in-ten adults incorrectly believe that Medicare is the primary source of coverage for low-income people who need nursing or home care, but Medicaid is the primary payer-covering nearly two-thirds of all home care spending in the United States in 2023.
The 2025 reconciliation law is estimated to reduce federal Medicaid spending by $911 billion (roughly 14%) over a decade and may have broad implications for home care, including for the workforce, support for family caregivers, and states’ coverage of services. Over half of Medicaid spending finances care for people ages 65 and older and those with disabilities, the enrollees most likely to use home care and related services, and reductions of this magnitude will leave states with tough choices to raise new revenues or reduce Medicaid spending. The reconciliation law also established a new type of 1915(c) home care waiver for people who do not need an institutional level of care. Take-up of the new waivers is expected to be low given the cuts to federal Medicaid spending and requirements for states to demonstrate that new waivers will not increase the average amount of time that people wait for existing waiver services. This issue brief provides an overview of what Medicaid home care (also known as “home- and community-based services” or HCBS) is, who is covered, and what services were available in 2025. Over 5 million people receive Medicaid covered home care services annually.
This brief is one of several describing data from the 23rd KFF survey of officials administering Medicaid home care programs in all 50 states and the district of Columbia (hereafter referred to as a state), which states completed between April and July 2025. Other issue briefs from the survey describe the number of people on waiting lists for home care, how states manage home care spending.States use various federal legal “authorities,” also known as programs, to offer home care, which are generally categorized as being part of the Medicaid state plan or part of a waiver. If services are provided through a state plan, they must be offered to all eligible individuals. In contrast, services provided under waivers, such as 1115s or 1915(c)s, may be restricted to specific groups based on geographic region, income, or type of disability. Waivers may include a wider range of service types than can be provided under state plans, but states may limit the number of people receiving waiver services. When the number of people seeking services exceeds the number of waiver slots available,states may use waiting lists to manage participation in the waiver.
All states have at least one home care program and many states have multiple programs. Home care is most frequently offered through 1915(c) waivers (47 states) and the personal care state plan benefit (33 states), and less frequently offered through 1115 waivers (15 states) or the Community First Choice option (10 states, Figure 1). KFF estimates that 5.1 million people used Medicaid home care in 2023 compared with only 1.4 million people who used institutional long-term care.
All states offer people assistance with self-care and household activities under the personal care benefit, but they use different programs to do so. the primary home care benefit is personal care, which provides people with assistance with the activities of daily living (such as eating and dressing) and the instrumental activities of daily living (such as preparing meals and managing medication). States most commonly cover personal care through waivers (48 states), followed by the state plan (33 states).
How are people eligible for Medicaid home care?
Most people who are eligible for Medicaid home care qualify on the basis of having a disability or being ages 65 and older. Medicaid eligibility pathways in which eligibility is based on old age or disability are known as “non-MAGI” pathways as they do not use the Modified Adjusted Gross Income (MAGI) financial methodology that applies to children, pregnant individuals, parents, and other non-elderly adults with low incomes. In addition to considering income and age or disability status, non-MAGI eligibility pathways usually require people to demonstrate that they have limited savings and other financial resources (e.g., assets). Because nearly all non-MAGI pathways are optional, eligibility levels vary substantially across states.
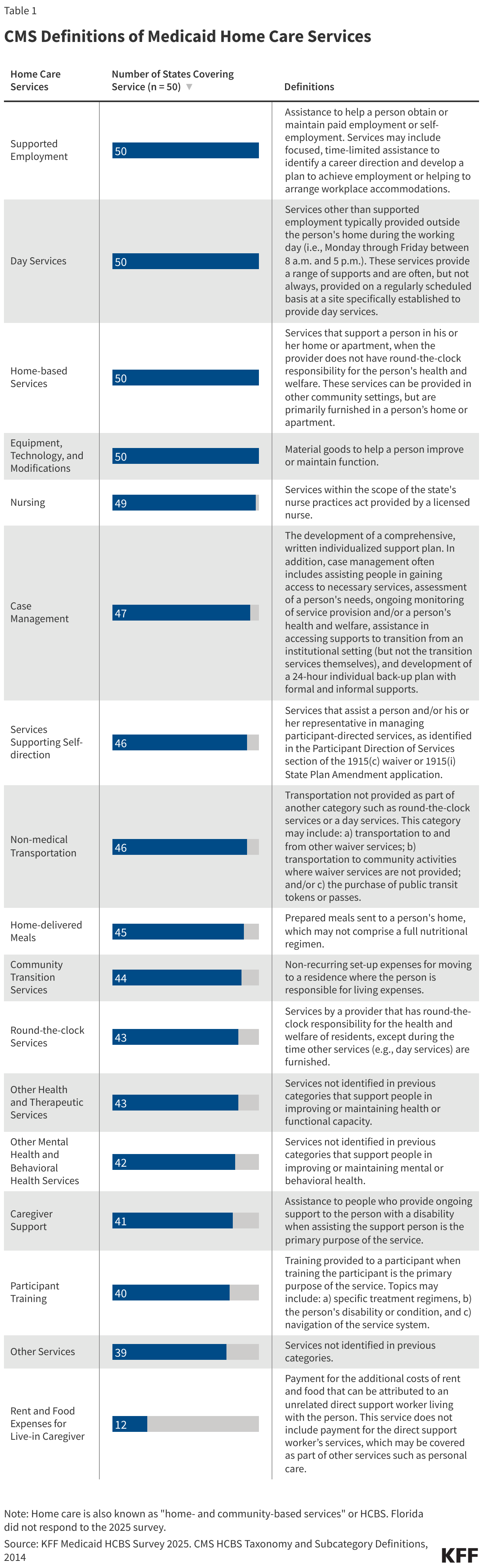
All responding states (50) cover supported employment, day services, home-based services, and equipment, technology, and modifications in any home care program (Appendix Table 3).States often also offer other additional services for specific populations that are uniquely tailored to the needs of waiver recipients. Examples of such services reported in the 2025 survey include:
- Illness support, group counseling, and bereavement counseling in a waiver for children who are medically frail or technology dependent (Colorado);
- Finding and career planning, additional residential supports, and community navigators in a waiver for people with intellectual or developmental disabilities (Hawaii);
- Dental services, permanent supportive housing, and prevocational/community career planning in a waiver for people with intellectual or developmental disabilities (Louisiana);
- Other speech, hearing, language, occupational, and physical therapies in a waiver for people who are ages 65 and older or have physical disabilities (Texas).
Among the categories defined by the Centers for Medicare & Medicaid Services, the least-frequently covered service was rent and food expenses for a live-in caregiver. For the most common services, there is little change in the number of states offering each type of service in a given year. (The numbers reported for most services are higher in 2025 but in many cases, that reflects a higher state response rate in 2025 than in 2024.)
States use waivers that target specific populations to offer tailored benefits, and covered services differ among different types of waivers (Figure 3, Appendix Table 4). Some services, such as equipment, technology and modifications, home-based services, and day services, are covered by most states and in most waiver programs. However,other services are much more targeted to specific populations. Comparing services among the most commonly-offered waivers (those serving people with intellectual or developmental disabilities and people who are ages 65 and older or have physical disabilities), shows some services are widely covered by one type of waiver but not the other. For example, 47 states cover supported employment for people with intellectual or developmental disabilities, but only 15 cover the service for people who are ages 65 and older or have physical disabilities, a population less likely to be working. Alternatively, home-delivered meals are covered by 41 states under waivers serving people who are ages 65 and older or have physical disabilities, but only under 10 states’ waivers serving people with intellectual or developmental disabilities. By enabling states to cover,at times,different services per target population,waivers allow states to customize services to the needs of the specific popu
PHASE 1: Adversarial Research & Freshness check – Medicaid Home Care & Managed Care (as of 2026/01/11 09:57:00)
Original Text Summary: The provided text discusses the increasing use of managed care organizations (MCOs) in delivering Medicaid-funded home and community-based services (HCBS). It highlights that most states utilize MCOs for at least some home health services, particularly those delivered through state plan benefits or 1115 waivers, but less so for 1915(c) waivers, especially those serving individuals with intellectual or developmental disabilities. The text also notes a trend towards greater predictability in Medicaid spending and service coordination as reasons for this shift.
Verification & Updates:
- Managed Care & Home Care Prevalence: the claim that “all but 11 states provide some Medicaid home care through managed care plans” is generally consistent with current data. A 2023 report by KFF (Kaiser Family Foundation) found that as of July 2023, 38 states (including DC) contracted with managed care organizations to deliver some level of HCBS. This aligns with the original text’s implication of 39 states utilizing managed care for home care (50 states – 11). https://www.kff.org/medicaid/issue-brief/managed-care-in-medicaid-a-primer/
- Capitation Payments: The description of capitation payments as a set fee paid to mcos per enrollee is accurate and a standard practice in managed care arrangements. https://www.cms.gov/medicaid/managed-care/capitation
- Growth Over Time: The statement about the growing use of managed care for Medicaid HCBS is also supported by data. The trend towards increased managed care penetration in Medicaid, including HCBS, has been ongoing for over a decade, driven by cost containment and care coordination goals. The linked PDF from Medicaid.gov (ltssexpenditures2020.pdf) is outdated. More recent data from CMS shows continued growth in managed care enrollment in Medicaid and CHIP. https://www.medicaid.gov/medicaid/managed-care/index.html
- Waiver Types & Managed Care Use: The distinction between 1115 waivers, 1915(c) waivers, and state plan benefits regarding managed care utilization is accurate.1115 waivers, which allow states greater versatility in Medicaid program design, are more frequently linked to managed care arrangements than 1915(c) waivers, which focus on specific populations (like individuals with intellectual/developmental disabilities) and often involve more specialized care models. The lower utilization of managed care for 1915(c) waivers serving individuals with I/DD remains consistent with current understanding.
- 2024 Data Point: The text mentions “4 more states than in 2024” using managed care for 1915(c) waivers. This is a specific data point that requires further inquiry. While the overall trend is towards increased managed care, pinpointing a precise increase of “4 states” between 2024 and the time of the original text’s publication (likely late 2023/early 2024) is difficult without knowing the exact date of the original source.KFF data from July 2023 shows 26 states utilizing managed care for 1915(c) waivers. As of January 2026, this number is 28 states. https://www.kff.org/medicaid/issue-brief/managed-care-in-medicaid-a-primer/
Breaking News Check: As of January 11, 2026, there are no major breaking news events substantially altering the landscape of Medicaid managed care and home care delivery.Ongoing legal challenges to specific state Medicaid waivers exist, but these do not represent a systemic shift in the overall trend.
Latest Verified Status: The information presented in the original text is largely accurate and reflects the ongoing trend of increasing managed care penetration in Medicaid-funded home and community-based services. The specific data point regarding a “4 state” increase between 2024 and the original text’s timeframe is partially verified, with an increase of 2 states observed as of January 2026. More recent data from KFF and CMS confirms the continued growth of managed care in Medicaid.
PHASE 2: Entity-Based GEO (Not Applicable)
This phase is